How Long COVID has become the ‘silent pandemic’

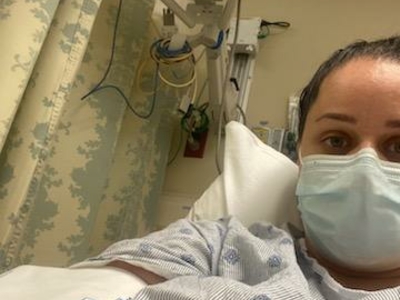
Every night at 5 p.m., Sheila Decker wraps up her full-time job and opens her computer to spend her evening hours reading “all the newest articles, the newest studies, the newest anything to gain knowledge of what’s going on” about Long COVID.
For almost two years, Decker, a 37-year-old living in the Lansing area, has gone on what seems like a wild goose chase to find any morsel of information about what her life has become: a neverending slog through countless COVID-19 symptoms.

When Decker first got COVID in April 2020, she found herself facing “crazy fatigue and gastrointestinal issues,” but the worst symptoms didn’t begin until a couple months after that: the increasingly debilitating exhaustion, the blurred vision, a heart rate of 160 beats per minute (a normal heart rate is between 60 and 100), and the headaches that left her with a pain she’d never before felt, as though “my brain was a balloon and it was getting bigger and bigger.”
“I remember my fatigue being so bad that it felt like I wasn’t going to wake up,” Decker said. “I was scared to go to sleep. I wear a Fitbit, and I gave my mom my log-in for my Fitbit because she works third shift and is up all night. I said, ‘Keep an eye on it and make sure I make it through the night.’”
Now, it’s been two years since the world plunged into a pandemic that has infected about 78.3 million people in the United States and killed close to 1 million Americans and more than 30,000 Michiganders, and Decker is still suffering from COVID symptoms. She’s gone to countless doctors — “every kind of specialist you can think of” — but she has gotten few answers about the pain now dominating her life.
“My health is different every day,” she said. “ A couple weeks ago I was questioning how much longer I’m going to be here because I was so symptomatic. Then, last week, I felt OK. It’s really random. A lot of the time, my symptoms are so uncomfortable. It’s hard to work. It’s hard to sit up. It’s hard to eat. Mentally, it’s a big cost. You’re just sick all the time, and you’re watching everyone around you live their life — and you wish you could do those things, too, but you can’t.”
‘A silent pandemic’
Decker is, according to public health experts, among a population of potentially millions of Americans suffering from Long COVID — a chronic illness that leaves individuals living with a wide variety of often debilitating COVID symptoms for months, or even longer, past their original COVID diagnosis.
Anywhere between 10% and 35% of those who have had the virus go on to develop Long COVID, with those numbers varying in part because there’s no universal definition of the illness, public health experts explained. Those hospitalized with severe COVID cases have so far been more likely to have long-term symptoms, although experts told the Advance there’s no shortage of people with originally mild COVID cases and younger individuals who are living with Long COVID.
“Individuals hospitalized with more serious disease, or should have been hospitalized but could not because of the crunch of the health care system — anywhere from 20 to 30% of those people may go on to develop Long COVID,” said Charles Downs, a Long COVID researcher and an associate professor at the University of Miami School of Nursing and Health Studies.
“We’re talking about a silent pandemic that could be in the millions of people who are affected,” Downs said.
Because Long COVID has become so prevalent, the Michigan Department of Health and Human Services (DHHS) stopped reporting data on so-called “recovered” COVID patients in January. DHHS explained that originally, the state categorized a “recovered” individual as someone who was alive 30 days past the onset of their COVID case.
This categorization changed to reflect the fact that while someone may be a month past their COVID diagnosis, that doesn’t mean they have fully recovered, DHHS said. In other words, because someone does not die does not mean they have recovered and may instead be suffering from Long COVID, the department stated. But, in part because Long COVID is not “identified from current case surveillance methods,” those recovery numbers can no longer be accurately reported.
Long COVID patients interviewed by the Advance wove a narrative that’s being told across the country, and world: one of never-ending sickness that’s left them unable to work and facing financial ruin and dealing with extreme frustration over medical and government landscapes that have often been unreceptive to their needs. They described overwhelming physical and mental health challenges that have caused many to repeat a similar sentiment: they feel hopeless. People are losing jobs and homes, being forced to sell homes in order to pay bills, and watching their young children have to care for them as they’re unable to move in bed.
“Every once in a while I get to that point where it’s like, ‘Why am I even going through this? Is this the way the rest of my life is going to be?’” said Deana Zepeda, a 65-year-old Davison resident who got COVID in June 2020 and still has such symptoms as extreme fatigue, shaking and breathing difficulties. “When I start talking like that, my husband gets upset and says, ‘You just have to keep fighting.’
“But what kind of life is this? It feels like what a terminally ill person would feel on really bad days, like there’s no hope. Why even live? You can’t do anything. Some days I don’t even want to eat.”
I remember my fatigue being so bad that it felt like I wasn’t going to wake up. I was scared to go to sleep.
What exactly is Long COVID?
Beyond the acknowledgement that a large portion of the population is dealing with COVID symptoms long after an original diagnosis, there’s still much that needs to be understood about Long COVID, researchers explained.
Public health experts noted they have yet to come up with a universally recognized definition of the illness, and there are no evidence-based treatment options yet. Doctors working with Long COVID patients are currently largely focused on how people can live with their symptoms.
It’s also unclear what causes Long COVID. Researchers have pointed to the severity of a COVID illness and whether someone has been hospitalized, asthma, obesity, and Type 2 diabetes as being some of the factors that seem to make it more likely for someone to have Long COVID — though, again, that’s far from clear at this point.
Research into Long COVID is certainly happening — the National Institute of Health (NIH), for example, in 2021 dedicated $1.15 billion to studying Long COVID. The University of Michigan and the DHHS also have partnered on the “Michigan COVID-19 Recovery Surveillance Study. The study includes more than 3,500 interviews with Michiganders at least 60 days after their COVID diagnosis in an effort to understand the impact of the virus and recovery from it.
But, experts emphasized, research is typically slow going, and public health experts certainly understand there are many people hurting now who aren’t getting answers about the Long COVID that has turned their lives upside down.
“Research is a slow process; it takes time,” Downs said. “These are human lives we’re talking about. Scientists tend to err on the side of being cautious anyway and want to be more cautious with people’s lives.”
I’m now at the point where I have no resources coming in. My bills are going unpaid, I can’t afford my medications, and I can’t afford to put gas in my car to get to my doctor.
Even with the $1.15 billion from the federal government, far more research funding is needed to study Long COVID across the country, Downs said.
“We need major research initiatives,” he said. “NIH has launched a Long COVID initiative. We need more of that, and we need it in ways in which the research could be done in a nimble fashion. The government acknowledging this and doing something is not a small thing, but at the same time it is the government and the government is not nimble or quick to respond to some of this.”
To address the concerns of the potentially millions of people with Long COVID, Downs said it’s critical for health experts to “get on board that there is a problem, what that problem is, how it develops, and how we can test and screen for it.”
Long COVID could also end up being a number of different syndromes currently lumped into one, as patients have described a wildly vast array of symptoms, those symptoms’ duration and their resolution (if there is any), explained Jana Hirschtick, an assistant research scientist at the U of M School of Public Health who’s been working on the Michigan COVID-19 Recovery Surveillance Study.
According to a 2021 study from Hirschtick and other U of M researchers — which found 35% of its participants were reporting Long COVID symptoms 60 days after the virus’s onset — the major symptoms reported by Long COVID patients were extreme fatigue, shortness of breath, persistent loss of taste or smell, and cognitive dysfunction, often colloquially referred to as “brain fog.”
While these seem to be the most prevalent symptoms, the Long COVID patients’ symptoms is a vast list. Additionally, some patients have seen their symptoms, or some symptoms, mysteriously vanish while others have had new symptoms arrive or their condition worsen, and others have continued to have the same symptoms since getting COVID.
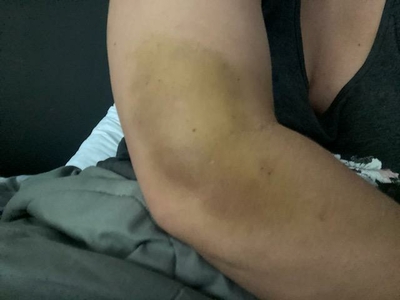
Of the Long COVID patients interviewed by the Advance, symptoms ranged from debilitating fatigue that left people unable to work to unrelenting headaches, heart palpitations, tremors, rashes, skin discoloration, and much more. One woman reported having 85 Long COVID symptoms over the past two years.
‘We can’t afford our medications; we’re not working; we don’t have money to get to our doctors. What do we do?’
For those with Long COVID, the symptoms are far more than words in a study: They are the reasons their lives have been upended. They’re the reason they’ve had to leave their dream jobs and stopped seeing friends and family. They’re why they can’t pay their bills or why they’re living on disability checks providing them with less than $200 a month.
These symptoms — this flood of fatigue, these skull-crushing headaches, this inability to breathe or move — are why they’ve spent days, weeks, months, and, now, for some, almost years in bed.
They have persisted. They have gone to doctor after doctor; they’ve scoured academic studies; they’ve connected with people around the world who, like them, have few to no answers as to why this is happening. And when it all will end.
Karyn Bishof, the founder of the COVID-19 Longhauler Advocacy Project — a nationwide organization that’s working to expedite answers about, and treatment for, Long COVID — explained her symptoms have been so severe that she went from being a firefighter paramedic in Florida to being unemployed and suffering more than 85 different Long COVID-19 symptoms. Bishof contracted COVID in March 2020 while working as a paramedic.
“I’m now at the point where I have no resources coming in,” said Bishof, who, in her role through the advocacy project, works with Long COVID patients in Michigan and across the country. “My bills are going unpaid, I can’t afford my medications, and I can’t afford to put gas in my car to get to my doctor. That’s like so many of us. We can’t afford our medications; we’re not working; we don’t have money to get to our doctors. What do we do?”
“It’s such a struggle, being confined to my bed 85% of the time, and my 12-year-old son having to become the adult of the house,” continued Bishof, who noted she’s currently living on $158 in monthly cash assistance payments. “He helps with cooking, the laundry and all the household chores. He’s been phenomenal, but it pains me that he’s having to take on this role and losing out on things in his childhood. It’s a lot of mom guilt.”
Like Bishof, Carrie Morse, a 49-year-old from Pontiac, lost her job because of COVID — for her, it was a full-time position she had recently taken at a church. Now, she’s accessing about $200 a month through state disability benefits, which she noted is nowhere near enough to cover basic needs like rent and food.
After more than a year of people airing horror stories about Long COVID, it was recognized as a disability under the Americans with Disabilities Act (ADA) in July 2021. While that has allowed some people to access disability payments, many have cited difficulties receiving the benefits.
“I’m in the process of applying for Social Security disability; I’m working with an attorney on that,” Morse said. “But they said that takes 12 to 15 months. My hope is that in 12 to 15 months I’m better. I don’t know what people do in the meantime. My Michigan disability is $200 a month. That covers nothing.
“I’ve tried to access everything I’m eligible for, and I’m hoping there are some nonprofits that can help out with things like car insurance,” she continued. “I still have car payments, I have a cell phone, electric, gas. The bills don’t stop coming.”
The financial stress combined with being physically ill and feeling completely isolated as family and friends begin to venture into the world again has been “completely overwhelming,” said Morse, who said she’s now on food stamps.
“My parents are worried sick about me,” she said. “Everything in my life is a struggle. Physically, things are a struggle. Mentally, things are a struggle. Figuring out how to pay my bills is a struggle.”

In addition to standard Long COVID symptoms, Morse has fallen eight times since Labor Day.
“Nobody will say it’s because of COVID, but I didn’t have these problems before COVID,” she said. “It’s been so frustrating because nobody knows.”
Now, Morse, a two-time cancer survivor, said she’s “terrified of falling all the time, and especially with the snow and ice.”
“It’s a constant source of stress,” she said. “I can’t walk. Walking from one end of Costco to the other wears me out. The brain fog has gotten better, and the fatigue comes and goes. If I do too much in a day, the next day I pay for it.”
‘With every test, they’ll say, ‘Nope, you’re fine.’’
Like every other Long COVID patient the Advance interviewed, Bishof has been to an endless stream of doctors. And, as with almost everyone we spoke with, she has been told by some doctors that there’s nothing wrong with her physically — that her health problems are “psychosomatic.”
“When I was told [my symptoms] were psychosomatic, it was my second visit to a workers’ comp doctor,” Bishof said. “When I went to him, I brought him my binder of medical records. And because I brought him this binder, he literally wrote in my denial letter that bringing my binder of medical records shows mental illness.”
“Some of us have waited months to see a specialist and get weirdly excited that day is coming; we think, ‘Yes, we’ll get answers,’” Bishof continued. “Then they go to the doctor, and the doctor just gaslights them. Some people stop going to doctors because they can’t deal with that experience anymore.”
Decker said an emergency room doctor told her, “It’s just anxiety.”
“I had a doctor offer me morphine because I’m sure he just wanted to shut me up,” she said. “We are ignored by doctors; we don’t have doctors to dig and do the research on what’s wrong with us. I’ve been sent to so many specialists, every kind of specialist you can think of. And then they’ll just send me to other specialists.”

Attempts to find out what’s wrong with her have left her feeling despondent, Zepeda said.
“With every test, they’ll say, ‘Nope, you’re fine,’” Zepeda said. “It’s very frustrating, and I understand they don’t know everything yet, but don’t act like we’re all crazy. It’s basically changed my whole life. Believe me, nobody wants to make this up.”
Bishof said the same: if only, she said, this was happening because of anxiety. Instead, life is a nightmare from which she never wakes.
“It’s unrelenting headaches: a COVID headache is unlike any headache you’ve ever experienced,” she said. “It never goes away. There are the heart palpitations, the tremors, the internal vibrations, the discoloration, the rashes, the secondary infections, the complete fatigue. The unrelenting fatigue. No matter how much you sleep, it never goes away.
“The memory loss is terrifying,” Bishof continued. “Every long-hauler will tell you they’re dealing with this. I’ll be in the middle of a conversation, and I’ll lose the thought as it’s coming off my tongue. It’s reminiscent of Alzheimer’s, and it’s very scary. I will cry on the spot sometimes when it happens. I won’t retain new information unless I go over it again and again and again.”
This phrase — long-hauler — is one many of those with Long COVID use to describe themselves. It is particularly apt — this idea that not only are the symptoms seemingly never-ending, but they are a burden to be carried. They are the weight that keeps them pinned to beds and couches, to homes they describe as prisons.
“Things like taking a shower have become undoable every day,” Bishof said. “Things like driving my son to soccer, I can’t do it. Cooking a meal, I can’t do it. I have a hard time writing because of hand tremors. I wake up every day in such severe chronic pain that I can’t stand up straight.”
Long COVID changes your entire world, explained the Rev. Dr. Sarah Bailey, a pastor in Flint and a community engagement specialist with the University of Michigan. Bailey, who has worked extensively with Long COVID researchers at the University of Michigan, was first diagnosed with COVID in late October 2020 and has been suffering from Long COVID since then.
“I walk to the mailbox, and I’m out of breath; I’ve become more closed in, more at home,” Bailey said.
“The lingering shortness of breath and the fatigue are two things that are still with me — and this halted speech pattern I have now,” Bailey said. “I began to notice I was not speaking in a fluent kind of way. I’m an orator, so it was very noticeable to me. It’s been a struggle. Everything in my life has changed.’
‘I started crying, knowing I’m not crazy’
While there could be millions of people with Long COVID — and that population is expected to grow as long as the virus exists, health experts said — the experiences of those with Long COVID have been overwhelmingly isolating. In addition to the social distancing the general population has needed to do, individuals with Long COVID explained they have had to do that while battling extreme health conditions every day for months on end.
One of the things that has helped, they said, was connecting with others suffering from Long COVID online — such as the Michigan COVID-19 Long-haulers Facebook group, which is a part of the Covid-19 Longhauler Advocacy Project.
“Having people to talk to helps,” Decker said. “It’s hard to find people to talk to. With family and friends, we can tell them we’re sick, and we’re not doing good, and I don’t think anyone realizes the severity of those words. I think people think it’s no big deal, or we’re going to get better. People have no idea what it’s really like or how serious our diagnoses are post-COVID. It’s not always easy to find somebody to talk to or relate to.
“I definitely found some comfort in the Longhauler [Facebook] group; it made me feel like I wasn’t alone and there are other people fighting and advocating,” Decker said. “People are posting new articles, new studies. When I first got sick, it lifted a huge weight off my shoulders. It validated what I was going through and didn’t make me feel so alone.”
Zepeda shared the same sentiments and said she not long ago spent time over Zoom with fellow long-haulers from the Facebook group. Talking with others facing similar health battles made her collapse into tears. It was validation that these life-upending experiences are not in her head, she explained, and that her pain is real, and others know that.
With every test, they’ll say, ‘Nope, you’re fine. It’s very frustrating, and I understand they don’t know everything yet, but don’t act like we’re all crazy. It’s basically changed my whole life. Believe me, nobody wants to make this up.
“When I did the Zoom meeting and saw people’s faces come up on the screen, I started crying, knowing I’m not crazy,” she said. “There are things that would happen [with her health], and I wouldn’t tell anybody because I thought I was imagining it. But then I’d see somebody else had the same thing happen to them.”
For Bailey, talking about Long COVID has also been about breaking down the stigma around sickness.
“There’s a stigma that a lot of people have about talking about the long-term effects they have,” said Bailey, who’s also the CEO of the Flint-based nonprofit “Bridges Into the Future,” which assesses social determinants of health and connects women and children with necessary resources. “Everybody wants to show they’re better; they’ve conquered it. But they need to talk about the suffering. We can’t suffer in silence.
“Anything we keep a secret has the ability to be destructive; once you start talking about it, it starts to lose most of its power,” Bailey continued. “If we choose to stay silent, we choose to feed the fuel that keeps it going and doesn’t warn other people — warn them what they can do about it or let them know they’re not alone.”
‘This is not the end’: Living with Long COVID
While patients aired numerous frustrations over their Long COVID symptoms not being addressed in the medical system, health experts interviewed by the Advance emphasized that there are many researchers and providers who know Long COVID is real and are doing everything they can to relieve patients’ pain.
“There are many of us out here who believe this to be a real phenomenon, and people are actively working to try to understand it,” Downs said. “We believe you.”
Dr. Thomas Hordt, a physician at Mary Free Bed Rehabilitation Hospital in Grand Rapids noted there are also clinics doing in-depth work with patients to help them be able to live again — to be able to work, spend time with friends and family, and generally function with Long COVID.
At the Mary Free Bed outpatient recovery program, which is located in Grand Rapids and at satellite sites around the state, Hordt said staff are working with patients for an average of six to 10 weeks on issues like chronic pain management and mental health. Of those in the program, about 75% of the patients end up returning to the workforce. Through the recovery program, individuals with Long COVID work with a variety of specialists on managing their symptoms with physical, occupational and speech therapies, Hordt explained. Patients will also spend time in group psychology sessions.
“A lot of these patients feel very isolated,” Hordt said. “Not many people know others going through these hardships. It shows them they’re not one of one but one of thousands dealing with similar symptoms.”

To help patients deal with their symptoms, Hordt said they will focus on “mindful techniques, coping strategies for symptoms.”
Hordt also works with patients to begin reentering the world.
“You have to engage in some activity; you can’t completely withdraw and that’s what we see in a lot of patients — a complete withdrawal from work, from social interactions they enjoy. As you withdraw and isolate, you’re feeding whatever underlying mood disturbance there may be — depression, anxiety. Now you’re more depressed; all you can do is sit at home and focus on your symptoms. We need to intervene with that.”
Ultimately, Hordt wants those with Long COVID to know “there is a light at the end of the tunnel.”
“You’re going to improve,” he said. “This is not the end; this is not the new normal for you. Things will improve.”
‘The impact will be enormous for communities of color’
As has been the case with so much of the pandemic, marginalized communities and people of color are being deeply impacted by Long COVID. Again, because of limited research, the full impact of Long COVID on people and communities of color is not fully known, but health experts said it exists and must be addressed as the pandemic continues.
“There’s all of these Long COVID advocacy groups, and the resounding message from those groups is they need to be heard and believed; that was a huge barrier in even getting recognition that Long COVID exists,” Hirschtick said. “People in these advocacy groups can be of higher socioeconomic status. If they’re having issues being believed and treated, the impact will be enormous for communities of color.”
A 2021 study from University of Michigan researchers showed Hispanic adults in Michigan had a greater prevalence of Long COVID than white individuals — 56% of Hispanic adults had COVID symptoms at 60 days past their diagnosis, compared to 34% of white adults. And according to the most recent report from the Michigan COVID-19 Recovery Surveillance Study, one in three Black Michiganders reported a mobility disability after their COVID-19 illness. Meanwhile, 13% of white Michiganders reported the same.
“To have this level of disability after infection is going to be a problem, not just for the individual, but for the medical system and the health care system and the public health system at large,” Nancy Fleischer, an associate professor of epidemiology at the U of M School of Public Health, said in a statement. “Even though we’re still focused on wave after wave of infections, we are going to have to deal with wave after wave of consequences for long-term health, including disability.”
To address these kinds of racial disparities, Hirschtick said there needs to be intentional funding for communities of color dealing with Long COVID and a focus on access to care.
“We need to make sure existing [health care] infrastructure for communities of color have the funding to create” Long COVID resources, she said.
Bailey, the pastor from Flint who has been dealing with Long COVID, said her city — a majority Black community — is facing the collision of Long COVID and systemic racism. The two are inextricably intertwined because institutionalized racism in everything from health care to food access left Black Michiganders and Black Americans more likely to contract COVID-19 and less likely to be able to access care before, during and after the illness, Bailey explained.
To truly deal with Long COVID, she said we must take a hard look at the institutionalized racism that exists in the medical world — and throughout our society, she said.
“Here’s a group of people that systemically, historically, generationally have not been treated well when it comes to medical attention,” she said. “What has changed? Nothing. That means Long COVID is a thing within a thing — it’s wrapped up within racism itself.”
And, she said, Long COVID is prevalent in communities of color like Flint because “so many African Americans were exposed to COVID because they had no choice. They had to go to work.”
“Once the pandemic hit, we called them essential workers; before that, we wouldn’t even pay them a decent wage to live,” Bailey said. “Until we deal with the ills we’ve created related to racial disparities, it’s going to be difficult to fight any kind of disease because they go hand-in-hand.”