Hoosier Medicaid recipients report higher program dissatisfaction than peers

Satisfaction rates for Hoosier Medicaid recipients trail behind the national average, with many delaying necessary medical care as low reimbursement rates disincentivize providers from accepting the coverage.
The findings come from a new national ‘Medicaid Matters’ report shared with the Indiana Capital Chronicle.
Over two-thirds, 71.8%, of national respondents were mostly or completely satisfied with the quality of care they received. But that number drops to three-fifths for Hoosiers, or 61.7%, who were mostly or completely satisfied. Even for those who enrolled successfully, the process was confusing and burdensome.
“… it was very easy to qualify for Medicaid by income because our income was clearly low enough. It was still a huge hassle,” said Anna Lisa Gross, a pastor at a Fort Wayne church, about her and her husband’s experience. “I also have a housing allowance usually… and whether or not Medicaid counts that as part of my eligibility, no one has been able to answer.”
Three national organizations — the Center for Popular Democracy, Make the Road New York and People’s Action Institute — surveyed nearly 3,000 Medicaid recipients between September 2022 and February 2023 about their experience in ‘Medicaid Matters: Challenges States Should Watch Out for as the Public Health Emergency Ends.’
The participants lived primarily in 14 states, including Indiana, but spanned the country geographically and politically – from California to Missouri and New York to West Virginia.
Nearly half of Indiana participants – 48% – said applying for Medicaid coverage was challenging while nearly 43% said they had difficulties attempting to renew their coverage. This comes at a time when millions of people across the country – including hundreds of thousands of Hoosiers – will suddenly lose coverage through a “redetermination” process.
The agency overseeing Medicaid, the Family and Social Services Administration (FSSA), noted that all states are navigating an unprecedented process and following federal guidance to resume normal operations. The department said it was “doing more outreach than ever before to reach Hoosiers who may be at risk of losing coverage.”
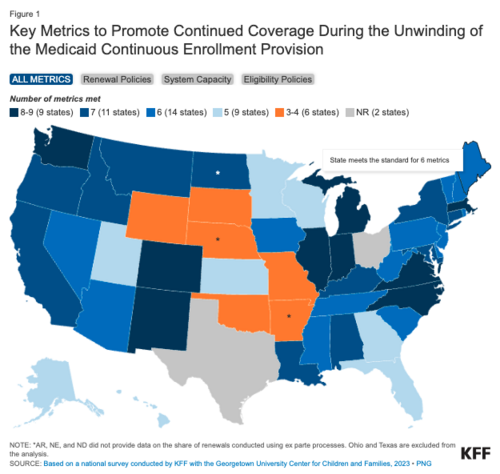
FSSA added that KFF, a non-profit health policy organization, ranked Indiana among the most prepared states for the redetermination process, crediting the agency for its renewal, capacity and eligibility policies.
“Throughout the process of returning to normal we have worked closely with Hoosier Action and other key stakeholders to help shape our approach and to get feedback from their members,” FSSA said in a statement. “Additionally, Indiana has taken several steps in recent years to improve Medicaid coverage. This includes extending post-partum coverage to 12 months, passing into law continuous eligibility for children and eliminating the 5-year waiting period for lawful resident immigrant children and pregnant and postpartum individuals. We have also taken steps to increase access to providers, including increased reimbursement rates.”
FSSA noted that the Indiana survey included just 129 Medicaid recipients but acknowledged that it provided “important, real life examples of what members face” while using the insurance program.
The report
Gross, whose interview was shared in a supplemental report from the advocacy group Hoosier Action, said she had no idea about how the redetermination process would work with her irregular paychecks and housing allowance. Additionally, she was one of many Hoosiers who said they struggled to find providers who accepted the government insurance program.
Nearly two-thirds, or 65.3%, of Hoosiers said they had trouble accessing services – specifically finding someone who had open appointments. Gross said, in her experience, the online insurance portal was simply inaccurate and didn’t reflect which providers actually accepted new Medicaid patients.
Heather Maritano, a mental health provider in Bloomington, told the report’s authors that dealing with Medicaid was like playing “insurance cat and mouse” and took time away from patient care.
“So if you take traditional Medicaid your reimbursement rate is going to be about half to a third of what the going rate is,” Maritano said. “… the reimbursement rates are lower, the systems are more difficult to navigate… (and) you have to hire extra support or spend more time (on it) yourself.”
Even for those covered, the remaining challenges discourage Medicaid recipients from seeking medical treatment – something 42.5% of Hoosiers said they did in the last year.
Gross said Medicaid, through insurance giant Anthem, only partially covered a series of surgeries she had in 2020. After applying for financial aid at IU Health, the state’s largest hospital network, she received a letter saying her medical debt would be canceled.
“I was happy to the point of tears. I would be able to breathe and focus on important matters,” Gross said. “Shortly after that, I received a letter from Harris and Harris, a debt collection agency. I was informed that I had an outstanding debt of nearly $5,000 with IU Health from Anthem for these first three surgeries. Double what I had even known.”
Roughly one in three Hoosiers rely upon Medicaid, according to a presentation from FSSA earlier this month. Those enrollment numbers swelled during the pandemic due to a federal provision to maintain continuous coverage throughout the public health emergency, which expired on April 1.
In exchange for the enhanced federal match, Indiana and other states vowed not to let anyone’s coverage lapse — even if their financial fortunes improved.
Following the expiration of the rule in April, states could start removing people from their rolls – which meant that nearly 53,000 Hoosiers lost coverage starting May 1. The first wave of an estimated 300,00-400,000 Hoosiers who might fall off the rolls after receiving continuous coverage for over three years.
Nationally, an estimated 17 million people could lose Medicaid coverage – many of whom are still eligible, according to KFF.
Roughly one-third of Hoosiers surveyed in the Medicaid Matters report, 34.7%, said they were unaware of the need to renew.
When faced with concerns about the numbers of Hoosiers dropping off of the rolls, FSSA leaders said that Hoosiers had 90 days to reapply for benefits with retroactive coverage – unless they were enrolled under the Healthy Indiana Plan 2.0 (HIP) which doesn’t allow for retroactive coverage.
Author recommendations
The report concluded with several sets of recommendations for both federal and state governments. On the national level, emergency Medicaid coverage should carry over – even for those people who no longer qualify following the end of the public health emergency.
Additionally, more funding should be dedicated to navigator and outreach programs, which the authors argued would help solve communication issues. Targeted outreach programs could be incentivized to find those with substance use disorders, which impacts roughly 12% of all adult Medicaid recipients.
The report found that groups who had support through the process had less challenges in applying or renewing. Authors emphasized the need to communicate clearly, especially for those with limited literacy or language barriers.
Other federal recommendations seem unlikely, such as Congress passing Medicare for All or expanding access to all immigrants regardless of immigration status.
But one suggestion that would target Indiana, specifically, would be a suggested federal requirement for states to increase their reimbursement rates for Medicaid providers. As stakeholders battled out the cause of Indiana’s high health care costs in the recently ended legislative session, nearly everyone agreed that the state didn’t pay enough for Medicaid providers.
First month of Medicaid ‘unwinding’ boots nearly 53K Hoosiers from coverage
In response, lawmakers included a provision in the budget to create an interim study committee to analyze the issue and compare Indiana’s Medicaid reimbursement rates with other states. Following the “equalization” of reimbursement rates, some providers will see increases in the coming months, as passed by lawmakers last month.
Other state-specific recommendations included designating an “unwinding czar” to coordinate with community outreach programs and hiring sufficient staff to reduce wait times.
“If staff recruitment is a problem, raise wages for call center and other agency workers (emphasis in the original),” the report said.
In terms of call wait times, more than two-fifths of Hoosiers, 44.1%, reported long call wait times when attempting to navigate application or renewal challenges – the third-highest rate in the nation.
Some country-wide respondents reported waiting on the phone for up to 11 hours behind 187 other callers.
Additionally, renewal and initial application processes could be easier and automated – reducing staff workload while easing the pathways for applicants.
The disenrollment of 53,000 Hoosiers, mostly for “procedural reasons,” demonstrates the need for Medicaid reform in Indiana, according to Tracey Hutchings-Goetz, the communication and policy director of Hoosier Action.
“Confusing notices, arbitrary rules and unnecessary red tape are fueling of potential crisis of uninsurance which threatens Hoosier health, the workforce and the future of our kids,” Hutchings-Goetz said in a statement. “… For over 2 million Hoosier kids, adults and people with disabilities, Medicaid provides the essential health care coverage we all need to get and stay well.”
Hoosier Action projected that more than 600,000 Hoosier Medicaid recipients could lose insurance coverage without action from FSSA, noting that other states saw smaller numbers fall off the rolls over the previous month and also reported fewer problems applying or renewing.
“We hope to work with FSSA and hope that they will take both swift action to reduce procedural disenrollments,” Hutchings-Goetz concluded. “As well as longer term changes to increase access to care.”








